BY MARY REINHOLZ | This holiday season has brought an uptick in respiratory illnesses for residents in New York and at least 17 other states, who have been afflicted with a range of ailments from flu and the common cold to outbreaks of COVID and RSV, according to the Centers for Disease Control and Prevention.
For the first time in my long and largely disease-free life, I was hit with RSV, respiratory syncytial virus or viral pneumonia. It’s an airborne malady that often strikes children and older adults, like this antique scribe from California, who had been previously misdiagnosed with sinusitis by a former primary-care physician and prescribed an antibiotic that was ineffective for RSV. A second primary-care doc prescribed another antibiotic after a brief phone consult, which also failed to wipe out my symptoms, including a headache, runny nose and a cough that turned into a volcanic rumble.
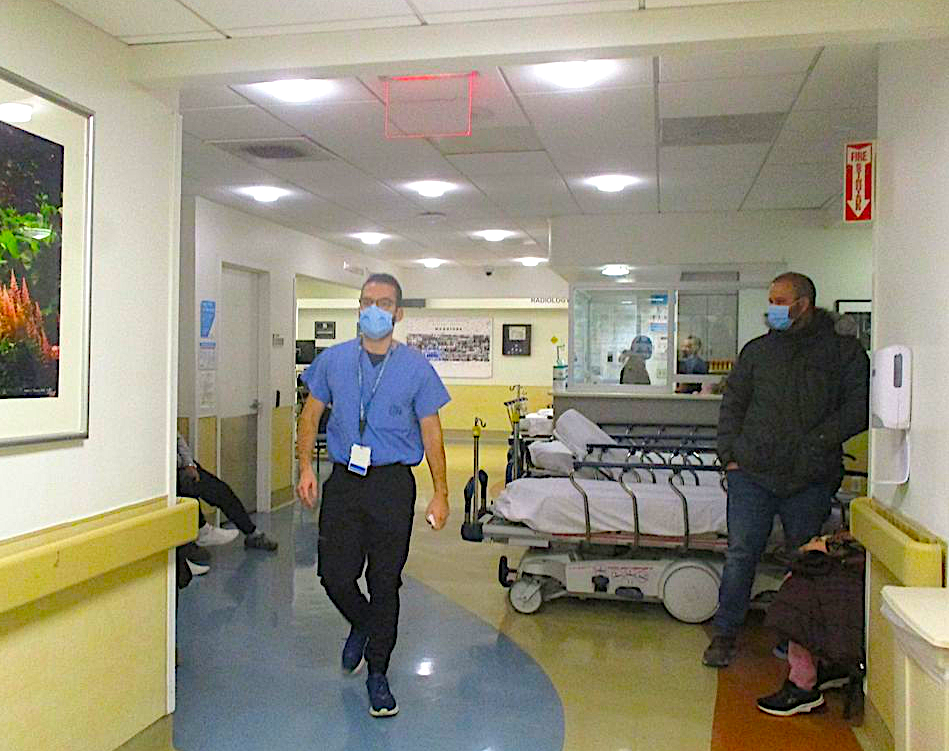
As it turned out, the award-winning emergency room at Beth Israel Hospital, run by Mount Sinai on E. 16th Street between First and Second Avenues, correctly diagnosed my virus and put me on a road to recovery in mid-December. Hopefully, this much-needed ER will remain open for other patients after July 12, when it has been slated for extinction along with parent Beth Israel Hospital, a 266-bed teaching facility founded in 1889.
As reported by The Village Sun, the Mount Sinai health chain claims Beth Israel and its ER have lost $1 billion over the last decade and are operating way below capacity. After an outcry from the community and a united front by outraged local politicians, including City Councilmember Carlina Rivera and state Assemblymember Harvey Epstein, the state’s Department of Health issued a cease-and-desist order to Mount Sinai on Dec. 21, declaring some of its recent shutdowns of beds and medical services at the Gramercy campus to be unlawful.
It’s unclear whether the D.O.H. order will push back or cancel Mount Sinai’s projected July closing of the Beth Israel campus, one of only two hospitals that serve thousands below 23rd Street in Downtown Manhattan. D.O.H. has yet to approve Mount Sinai’s closure plan.
Meanwhile, there seemed to be no shortage of patients when I first checked out the Beth Israel emergency room around 2 p.m. in early December: There were about 20 people ahead of me, waiting to be seen for its specialties, like cancer care and treatment for heart attacks and strokes, along with psychiatric emergencies.

About a week later, I returned at 11:15 p.m. and received immediate medical attention after blurting to a nurse: “I’m having trouble breathing.” I was gulping for air from my mouth and felt like there was a foot pressing against my chest.
These days, I’m breathing well through my nose, largely because of the competent and compassionate care I received over more than four hours during my long night’s journey at Beth Israel’s ER. Staff got me a curtained spot with a stretcher/bed, told me to put on a gown that tied in the back, inserted an IV, took blood and urine samples and conducted at least two exams of my chest with state-of-the-art technology.
Twice during this process, Dr. Robin D. Roberts, an emergency medical specialist, stopped by on his rounds, first announcing, “You’ve got a virus.” He was followed by Amanda Austin, a physician assistant, who explained RSV to me, noting, “It’s going around,” and talking in a casual, low-key tone about the disease, thankfully making me feel like I was not on a fast track to the morgue.
Another pleasant young woman came by to check out my insurance from UnitedHealthcare and ID from the New York Department of Motor Vehicles. She seemed to think there would be no problem for the ER to get paid for its services on my behalf. Cost for my visit will be a $90 copay through my insurance, according to representatives both at UnitedHealthcare and Beth Israel. The latter rep said that no patient is “ever turned away” from the ER without health insurance or aid in getting it.
A male nurse, who called himself Outback, kept monitoring a computer for updates on patients near my bed and twice led me by hand to one of the ER’s “all gender” bathrooms. Later, resting up, I listened to another medical professional talking to a much younger woman in a space next to mine who had an apparently serious illness. He asked her: “Do you live alone? Do you have a family? A husband? Anyone looking after you?” This jaded newsie finds such expressions of sincere concern rare in New York, including in doctors’ offices.
It was still dark outside after I was released around 3:40 a.m. with a 21-page summary of my visit, detailing my diagnosis, the meds I was taking and a statement urging me to return to the emergency room immediately should “new or worsening symptoms” occur. I would have walked out but Dr. Roberts suggested I stay around in a smaller room “until the sun comes up.” He was clearly worried that I might run into less-healing encounters on my way home a few blocks away in Gramercy.
As I was heading out the ER’s door that early morning Dec. 14 around 5:15 a.m., several EMS workers were coming in on the ramp, transporting an elderly Black man in obvious pain as he lay on a stretcher. It was a moment when I witnessed the raw power and medical resources of a great city come together to help another ordinary person in desperate need. I’m hoping that thousands of other people in Lower Manhattan will demand that New York State’s Department of Health require that Mount Sinai’s Beth Israel Hospital and ER remain in the neighborhood to continue a life-saving mission.
“The community has to come together to save the hospital,” said a cardiologist at Mount Sinai’s ambulatory facility at 10 Union Square East who examined me some 48 hours after Beth Israel’s ER released me, requiring that my current primary-care physician or another physician check me out within that time frame. The primary-care doc e-mailed me the name of a “specialist” three days later, but the cardiologist had my blood pressure and pulse taken on time.
He also examined the meds I had been prescribed by the ER, including a breathing mechanism for inhaling sprays of aerosol and wrote back to Beth Israel on his computer.
“You should be O.K. in four days,” he predicted. It could take longer but I seem to be doing well enough, thanks to a beloved institution in my neighborhood that’s now in more peril than I am.


Beth Israel used to make money for its former owners. Mount Sinai removed most of the profitable services and sent them to other sites. Now they claim the hospital is losing billions. It is by design. The most profitable thing about the hospital is the real estate at this point. They are trying to close New York Eye and Ear too. Follow the money and watch as they pay politicians off to do what they want. They do not care about people or the health of the community.
Great story. My husband was born in that hospital. Wasn’t just two years ago that we did not have enough beds to treat the surge in COVID cases? In a city this size we have to have neighborhood hospitals.
I’m glad the writer is better. I’m curious if she had the RSV vaccine.
No, I did not and none of the four physicians I consulted even suggested that I get the RSV vaccine. Didn’t want to take up too much space in the article ranting about these docs, one of whom diagnosed me with rhinitis and another said maybe the dust in my Gramercy pad was contributing to sniffles and sneezing. Only Beth Israel’s ER diagnosed my RSV correctly and put me on road to recovery.
When I saw my doctor for my annual physical in October, she recommended I get the RSV vaccine, so I did.
You have a responsible doctor, congrats!
Thanks for your kind words. Local leaders in fight to save Beth Israel are the pols cited in piece, among them City Councilmember Carlina Rivera and state Assemblymember Harvey Epstein, plus healthcare unions like 1199.
With NYC having the worst congestion in the nation, Beth/Israel Mt. Sinai is sending patients Uptown to the monster campus. I had a friend who was sent up there — “the robots are more precise” than the human surgical hand. He died. He might have died anyway but he was maneuvered Uptown in part to demonstrate less Downtown need. With the congestion courtesy of Vision Zero — the bike lanes, the quieting zones and the lawless environment due to the lack of a responsible cycling/micro-transport culture — can anyone say “enforcement”? The chances of anyone surviving emergencies is seriously diminished if Beth Israel caters to the real estate developers and cashes out.
Are Downtowners considered so insignificant that the community is not considered worthy of adequate healthcare? Do we not pay rent? Are the real estate interests trying to kill off the sick and elderly? That would seem to be consistent with the last 23 years of virtually nonexistent enforcement against the rogue riders. New York City has always lagged in civility and culture behind Boston and Philadelphia, placing commerce above all else. This predatory
approach is unfortunately consistent with a bludgeoning of the quality of life and clearly the ability to “live.”
Beautifully written and moving article. As a resident of the Lower East Sice/East Village, I, too have relied on the Beth Israel emergency room and the hospital itself for my healthcare on many occasions. The next questions: what groups are active in fighting for the survival of our hospital and how can we get in touch with them and join in this incredibly important local struggle? Thanks! Fran Luck